Written by Aphelele Nodo
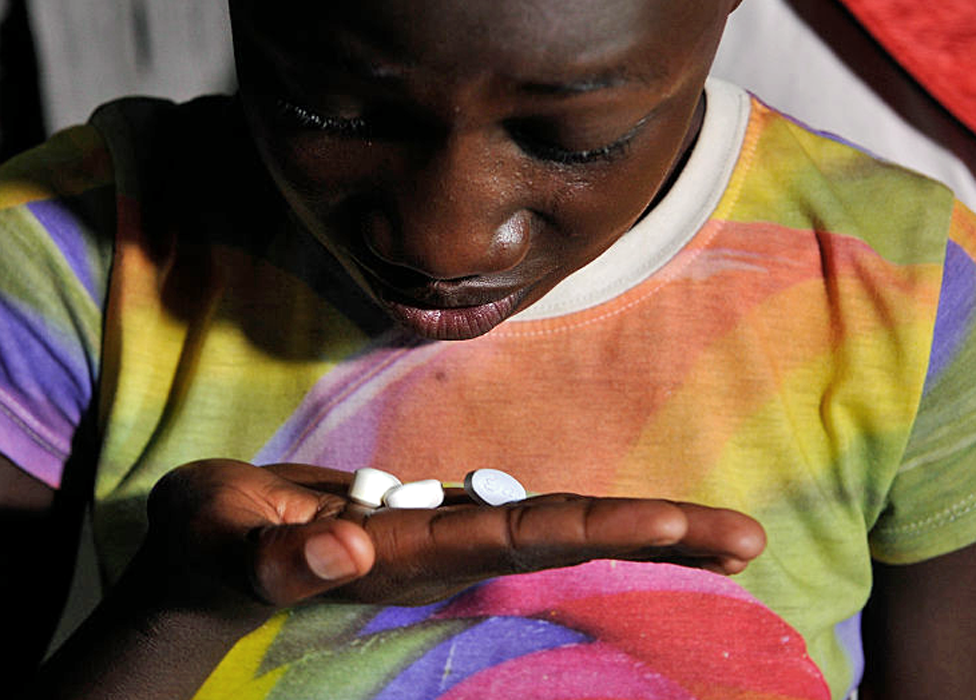
Recently, I was scrolling on social media when I saw an interesting post by an activist who is living positively with the Human Immunodeficiency Virus (HIV). In the post, she talks about the work that needs to be done to fight the spread of HIV and how young people are still getting infected with the virus at an alarming rate. She goes on to say that even though the government has done the work of providing medication and treatment to control the spread of the virus, and assist those living with the virus, there are still new cases. She specifically talks about the substantial number of children who were born with HIV through mother-to-child transmission through breastfeeding, pregnancy, and delivery. This often happened when antiretrovirals (ARVs) were not freely available in South Africa and before programmes to prevent vertical transmission was implemented.
Before antiretrovirals became available in 2003, there was a much higher rate of infection and transmission in South Africa. The availability of antiretrovirals together with the program for the prevention of mother-to-child transmission, led to a substantial reduction in infection and transmission. This provided evidence that when the ARV medication is taken properly (without defaulting) the viral load decreases to such an extent that the infected person has an undetectable viral load. This undetectable viral load substantially reduces the possibility of infecting someone else. Similarly, mothers who are living with HIV (but have reduced their viral loads with ARVs) can have children who are HIV-negative.
I thought about this in relation to my research study which seeks to explore parents’ narratives around appropriate familial conversations regarding young people’s (non)-use of contraception within a South African context. The research study is centred on parent-child interactions about contraceptives. While reviewing the literature I found that parents do not often have conversations about sex and contraception and when parents do have these conversations, they are coercive and centred around the idea that sex always results in danger and disease.
There are a limited number of parents who have informative and open conversations with their children. In the context of HIV-infection, communication is needed to support teenagers who trying to navigate life while living positively with HIV. For example, how does a teenager who is HIV positive, navigate the process of being in a relationship, disclosing their status and having sexual intercourse with or without protection? Some teenagers are not aware of their status because their parents have not disclosed the information. Parents struggle to initiate and counsel teenagers through a healthy process of disclosure. In this environment, nondisclosure can happen through dishonesty and deception by not being fully informed about the medication one is taking. Teenagers can get tired of taking medication and default. The lack of adherence increases their viral load and leads to potentially infecting others when they engage in sexual activity without protection.
Another issue that parents must understand is that the timing around disclosing HIV status to their children is vital. Parents have no way of knowing for sure when their teenagers will start with sexual experimentation. There are important conversations about sexual health that parents and guardians need to have with teenagers. Often parents are not only ignorant about their teenager’s activities but also believe the myth that talking about sex and contraception encourages premature sexual debut. In reality, parents who communicate with teenagers about sex and contraception can help to empower them, to protect themselves and their partners, when they are ready for sex. In the absence of these discussions, teenagers often use unreliable sources for important information about access to the different contraceptive methods available. Hence parents and guardians can be the most suitable people to engage in practical conversations to protect the teenager from defaulting on medication, from reinfection and from infecting others.
These conversations are not always easy but the alternative of ignoring the problem is much worse. Parents might need support from other professionals such as healthcare providers, social workers, or psychologists to encourage their teenagers to accept their status and not default on their treatment. It has been found that the trauma of late or non-disclosure exacerbates confusion and psychological distress for teenagers. When they find out that their parents or guardians have been dishonest and have kept their HIV-positive status a secret, it can cause a lot of damage to the relationship between the parent and the teenager.
Rather than parents contributing to this burden and making the situation much worse, they need to accept their responsibility of helping to equip teenagers to deal with the stigmatization, myths, and judgment, that people who are HIV-positive, often continue to experience in South Africa.
Kimani, S. (2019, July 3). 'My mother died without telling me I had HIV': BBC News. https://www.bbc.com/news/world-africa-48799980
